By Dipak Chudasama, BDS, MSC, MORTH, RCS, MBA, and Theodore Freeland, DDS, MS
The field of dentistry has seen significant advances in recent years, and orthodontics is no exception. But the issue of oral hygiene in orthodontics has remained a perplexing problem.
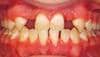
Patients seek orthodontic treatment mostly for esthetics issues even if they have functional occlusal problems. The orthodontist and parent or patient invests time, material, expense, and expertise to achieve beautiful smiles. When the day for appliance removal is finally reached, everyone from patients, families, and the treating orthodontist and staff are excited. However, the euphoria is short-lived when noticeable decalcification, in the form of white/brown spots resulting from poor oral hygiene during treatment, ruin the esthetic value of the case (Figure 1A).
 |
| Figure 1: (A) Decalcification and gingival infection post-treatment. (B) An example of poor oral hygiene pretreatment. This type of patient should not be treated until the gingival problems are rectified. |
Patients find it difficult to brush and floss around orthodontic appliances. This leads to a reduction in oral hygiene, which results in an increased risk for developing decalcification, decay, and gingival infections. The severity of the resultant dental caries can range from development of opaque white spot lesions (WSL) to the loss of surface integrity of enamel, cavitation and oral caries, and periodontal bone loss. As a profession, we need to focus on preventative measures and practices to improve oral hygiene and minimize adverse sequel to the teeth and periodontium.
Orthodontists should be aware of the high risk of WSL and decide, at the patient level, whether it is appropriate to start or continue treatment in patients who are already experiencing enamel demineralization and continual gingival inflammation. The risk of developing incipient caries and gingival lesions during orthodontic treatment should not be underestimated by orthodontists.
Research indicates that 49.6% of orthodontic patients exhibit enamel opacities on at least one tooth after orthodontic treatment. There is a significant risk that one in every 10 bonded teeth is likely to have post-treatment white spots with the incidence in banded teeth being slightly more at one in nine teeth. A significant increase in incidence, prevalence, and severity of enamel opacities following orthodontic treatment has also been reported in the same study.1
What follows are a number of responsible factors.
Factor One: Pretreatment Patient Assessment
At the initial exam, the doctor should perform a complete periodontal exam that assesses the health of the periodontium and the patient’s oral hygiene. If the oral exam shows plaque accumulation and gingival bleeding, then this patient should not be considered for orthodontic treatment until the gingival tissues are completely healthy (Figure 1B).
 |
| Figure 2: A toothbrush is used in place of a periodontal probe. This way, the parent/patient cannot accuse the practitioner of cutting the gums. |
Factor Two: How To Identify Oral Hygiene Problem Patients
With the toothbrush, the doctor places the bristles into the sulcus area in the anterior and posterior areas. If bleeding occurs, then there is a hygiene problem (Figure 2).
Factor Three: How To Improve the Patient’s Oral Hygiene
At this time, a preventative dental program should be introduced. If the patient still shows gingival bleeding after the program, then he/she should not be placed in orthodontic treatment. This program should be designed to enhance the diagnosis so the doctor and patient can discover the oral hygiene problems together.
The preventative program has five parts. The first two appointments are one week apart, and the proper techniques for oral hygiene are taught and reviewed. The next three appointments should show complete gingival health over a 3-month period. If this is not the case, then orthodontic treatment should be withheld from this individual. It is the responsibility of the orthodontist to withhold treatment, because if the patient will not take care of the teeth and gums before treatment, their oral hygiene will not improve during treatment.2
A close relationship with the referring dentist and his hygiene staff will facilitate the efforts of the orthodontist. Making sure the patient sees the dentist/hygienist more often may help reinforce the orthodontist’s efforts to obtain a disease-free mouth.
Factor Four: Oral Hygiene Problems During Appliance Therapy
Once treatment begins, the orthodontist is responsible for proper instruction on how to manage the hygiene issues created by the appliances. The doctor should demonstrate proper use of the brush and floss. If the doctor spends the time, it will impress on the parent/patient the importance of oral hygiene (Figure 3).3
 |
| Figure 3: (A) Flossing should be demonstrated, especially focusing on how the patient gets the floss into the sulcus. (B) Brushing needs to be taught to show how to get the bristles into the sulcus. |
The doctor should create an appliance environment that enhances the patient’s ability to care for the gingiva and enamel. All flash from bonding and banding should be removed. The use of sealants, such as Proseal, as part of the bonding procedure should be instituted. The bonding system should contain fluoride. The use of mechanics systems and retention systems that make it difficult to clean should be avoided. In light of the patient’s past oral hygiene issues during appliance therapy, bonded retainers should be avoided. As bonded retainers are placed “invisibly” on the lingual tooth surfaces, patient acceptance is evident. This practice may lead to the development of carious lesions, and favor the formation of plaque and calculus around the mandibular retainers, compared to the maxilla.7
Björn U. Zachrisson, DDS, MSD, PhD,4 one of the pioneers in the field of bonded lingual retainers, stressed the importance of daily interproximal cleaning with dental floss. Despite optimal oral hygiene instructions, calculus formed to a greater extent on the lingual surfaces of the incisors with bonded retainers, compared with incisors without bonded retainers.7
The patient is responsible for the care of the teeth and gingival tissues. If all efforts have failed and the oral hygiene does not improve, then the orthodontist should consider terminating treatment, even if it is a unilateral decision on the orthodontist’s part.
Laurance Jerrold, DDS, JD, explains that the doctor-patient relationship is bilateral and consensually based. He further elaborates that once in existence, this relationship can be dissolved in five ways: (1) both parties agree to end it (a common example is when the patient is relocating). (2) The patient’s condition is cured, and no further treatment is required. (3) The doctor or patient dies. (4) The patient decides to unilaterally terminate the relationship. Or (5), the doctor decides to unilaterally terminate the relationship.
Jerrold further elaborates by suggesting that the doctor can unilaterally terminate the relationship if the patient breaches at least one of the five duties owed to the practitioner under the contract that comprises the doctor-patient relationship: (1) the patient is not following the doctor’s instructions regarding treatment, and thus is jeopardizing his/her own treatment (Figure 4); (2) the patient is not keeping appointments, thus causing interruptions in the continuality of care, not to mention the interference with the business aspect of the doctor’s practice; (3) the patient is not being truthful or forthcoming regarding necessary administrative inquires (eg, their medical history, information about those financially responsible for care, their degree of cooperation, signs and symptoms of problems, and so on); (4) the patient is not conforming to accepted modes of behavior (he is belligerent or abusive to the doctor or his staff, or is creating a hostile or unhealthy environment in the office); and (5) the patient is not paying for services rendered.6
 |
| Figure 4: A case where the patient would not follow the oral hygiene program, so treatment was discontinued. |
In all fairness to the patient, some patients will exhibit gingival swelling in response to the appliances during treatment. It begins within a couple of months after placement of the appliances. Fixed appliances predispose plaque accumulation and colonization of bacteria. When gingival tissues are enlarged, the tooth surfaces/bracket tooth interface become difficult to access, inhibiting good oral hygiene and resulting in an increase in inflammation and bleeding. The interruption of orthodontic treatment is often advised when gingival enlargement is diagnosed. The temporary removal of the irritating factors, such as attachments and appliances, debridement, chlorhexidine prophylaxis, and, in some patients, surgical intervention such as flap/laser surgery to restore the contour of the enlarged gingival tissues, can facilitate adequate oral hygiene during subsequent orthodontic treatment.4
Conclusion
The benefits to the practice are enhanced in many ways, by having all patients’ gingiva disease-free while under orthodontic care. Increased patient referrals will occur because their cases are finished on time with a beautiful smile that is enhanced by healthy gingival tissues and teeth free of decalcification.6 Increased referrals from the dental profession will occur when their patients are being well taken care of while in the orthodontist’s practice. A study on marketing forces failed to discern or ascertain the degree/depth of the emotional connection created between the orthodontist and patient.5 This doctor-patient relationship is the most important aspect in finishing cases with healthy gingival tissues and free of decalcification.
The parent/patient will differentiate services offered by different practices. They will choose the practice that develops the bonds necessary to create the healthy oral environment. This will enhance the patient satisfaction at the end of treatment, even if the cases are walk-in/Google/patient-referral cases, because we will be judged by the general dentists at the oral hygiene appointments.
Other benefits to the practice are on-time finishes. A healthy oral environment always finishes on time. The esthetic value is always present, so at post-treatment consultations the parents/patients are most willing to refer their friends to your practice. The time spent trying to improve oral health is one of the best practice-building techniques, better than all the marketing techniques combined. OP
 |
Dipak Chudasama, BDS, MSC, MORTH, RCS, MBA, is in private practice in Coppell, Tex. He can be reached at [email protected]. Theodore Freeland, DDS, MS, is a past adjunct professor in orthodontics at the University of Detroit and director of the Advanced Education in Orthodontics Group. He is in private practice in Gaylord, Mich. He can be reached at [email protected]. |
References
1. Gorelick L, Geiger AM, Gwinnett AJ. Incidence of white spot formation after bonding and banding. Am J Orthod. 1982; 81:93-98.
2. Beckwith FR, Ackerman RJ , Cobb CM, Tira DE. An evaluation of factors affecting duration of orthodontic treatment. Am J Orthod Dentofacial Orthop. 1999; 115:439-447.
3. Yeung SCH, Howell S, Fahey P. Oral hygiene program for orthodontic patients. Am J Orthod Dentofacial Orthop. 1989; 96:208-213.
4. Zachrisson S, Zachrisson BU. Gingival condition associated with orthodontic treatment. Angle Orthod. 1972; 42:26-34.
5. Huges D, Landay, M, Straia S, Tuncay O. Application of a classical model of competitive business strategy to orthodontic practice. Am J Orthod Dentofac Orthop. 1996; 110:405-409.
6. Jerrold L. Problems of our own making: A view from both sides of the coin. Am J Orthod Dentofacial Orthop. 2012; 142-5:734-738.
7. Orsborn OB. Bonded lingual retainers. Am J Orthod. 1983; 83:218-220.